Elder Law Blog
Senior care blog covering topics like estate planning, asset protection, probate, wills, and trusts. Get the latest updates sent to your inbox today, by signing up for our weekly newsletter.
FEATURED
Early Action Can Prevent a Family Crisis
May 31, 2026 / Blog / Estate Planning / Life Care Planning

Estate Planning Mistakes That Can Cost Nashville TN Families Thousands
Key Takeaways Many estate planning mistakes are not discovered until a medical emergency, death, or probate dispute occurs. A will alone may not fully protect assets or help families avoid probate in Tennessee. Outdated beneficiaries, missing powers of attorney, and...
Protecting Your Home and Savings with Estate Planning in East Brentwood
Estate planning helps East Brentwood families protect their homes, savings, beneficiaries, and long-term wishes. A comprehensive estate plan can reduce probate complications and help loved ones avoid unnecessary court involvement. Wills, trusts, powers of attorney,...
How a Disability Attorney in Franklin, TN Helps Protect Your Benefits and Future
Key Takeaways A disability attorney in Franklin, TN, handles every stage of a Social Security disability claim, from the initial application through the appeals process. Social Security Disability Insurance requires enough work credits from your work history;...
What a Medicaid Planning Attorney Does for Nashville Seniors and Families
Key Takeaways: A Medicaid planning attorney helps families qualify for Medicaid while protecting assets and avoiding costly mistakes. Medicaid rules in Tennessee are complex, highly specific, and easy to misunderstand without professional guidance. Long-term...
Writing Your Will in Tennessee? Why Hiring a Last Will Lawyer Is Essential
Key Takeaways Tennessee wills must meet strict signing and witness rules DIY wills often lead to costly mistakes and disputes Estate planning lawyers provide personalized, legally valid documents Regularly update your will after major life changes Wills alone may not...
How to Find the Best Elder Law and Estate Planning Attorneys in Nashville, TN
Key Takeaways The best attorneys in Nashville, TN, combine legal skill with genuine compassion. Choose a lawyer who focuses on elder law or estate planning every day. Working with a local Nashville attorney helps you plan with Tennessee laws and resources in mind....
What Is a Medicaid Asset Protection Trust and How Does It Work in Tennessee?
Key Takeaways A Medicaid Asset Protection Trust helps families protect savings and property while meeting Medicaid’s asset limit for long-term care. Because it’s an irrevocable trust, any assets transferred into it must be planned well in advance. Tennessee has a...
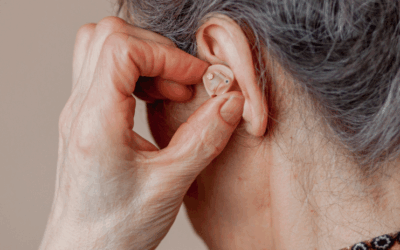
Hearing Loss and Dementia: How Early Intervention Protects Health and Independence
Key Takeaways Hearing loss is common in older adults and linked to a higher risk of dementia. Early diagnosis and treatment can help protect memory and mental clarity. Regular hearing evaluations after age 50 are essential for healthy aging. Untreated hearing loss can...
Are Children Responsible for Their Parents’ Debt After Death? A Guide for Nashville Families
Key Takeaways In Tennessee, children are not personally responsible for unpaid debts in a parent’s name alone. Debts are settled through probate and paid from the parents’ estate before any assets are distributed to the heirs. Children may only be liable for debts...
How to Prove Undue Influence in a Tennessee Will or Trust Case
Key Takeaways Undue influence occurs when someone manipulates a vulnerable person to change a will or trust. Proving undue influence requires evidence of control, pressure, or unfair persuasion. Tennessee law looks at relationships, suspicious circumstances, and...
Recorded Deed Notices: Protecting Yourself from Property Scams for Tennessee Residents
Key Takeaways A recorded deed notice helps confirm that your property ownership is secure. Scammers often target seniors with fake notices or fraudulent property filings. Tennessee homeowners can protect themselves by verifying official notices and monitoring records....
A Guide to Tennessee Veterans Benefits: What You May Be Missing
Key Takeaways: Many Tennessee veterans and their spouses are missing out on state and federal benefits to which they’re eligible. Available programs include VA healthcare, Aid & Attendance, and burial benefits. Surviving spouses may also be eligible for monthly...
Irrevocable Trusts Explained: Protecting Assets with the Right Legal Guidance
Key Takeaways: Irrevocable trusts can shield assets from long-term care costs and estate taxes. These trusts are not easily changed; professional guidance is key. An experienced irrevocable trust attorney helps ensure your wishes are protected. Families across Middle...
Paranoia and Cognitive Decline in the Elderly: What Nashville Families Should Know
Key Takeaways: Paranoia in elderly individuals may signal underlying cognitive decline. It can be caused by dementia, medication side effects, or loss of hearing or vision. Early legal planning can protect your loved one’s well-being and finances. Local attorneys can...
Estate Planning in Hendersonville, TN: How a Local Attorney Can Help
Key Takeaways: Estate planning is more than a will; it's about protecting your loved ones and your legacy. Local attorneys in Hendersonville, TN, are well-versed in state laws and understand the community's specific needs. Services may include wills, powers of...
Elder Abuse in Tennessee: What Families Need to Know
Key Takeaways: Elder abuse in Tennessee includes physical, emotional, financial, and neglect-related harm. Warning signs include mood changes, unexplained injuries, and missing money. Tennessee law requires certain professionals to report suspected elder abuse. Legal...
Planning Ahead: What a Wills and Trust Attorney Near You in Nashville, TN Can Offer
Need a wills and trust attorney near Nashville, TN? Learn how estate planning in Tennessee can protect your family, assets, and legacy with expert legal support.
Navigating Tennessee Medicaid for Seniors: A Step-by-Step Guide
Explore this guide by Elder Law of Nashville on Tennessee Medicaid for seniors. Learn eligibility, benefits, and how to apply.
Finding the Best Nashville Estate Planning Attorney: Protect Your Legacy & Loved Ones
You’ve undoubtedly been planning for the future your whole life, but there comes a time when such planning doesn’t include you in that future. Instead, such planning helps ensure the best for your family after you die. Estate planning ensures that your assets are...
Understanding Medicaid Eligibility in Tennessee: What You Need to Know for 2025
Elder Law of Nashville details what you need to know about Medicaid eligibility in Tennessee and how to navigate TennCare requirements.
Choosing the Best Elder Lawyers in Nashville: Key Factors to Consider for Your Family’s Protection
Finding an elder lawyer in the Nashville, Tennessee, area is as easy as typing “elder lawyer near me” into your Internet search engine. For a more comprehensive search, you can get listings of Nashville-area elder lawyers from any legal organizations that profile,...
Why You Need an Estate Planning Attorney in TN: Protecting Your Assets and Legacy
Estate planning is one of the most crucial steps you can take to ensure that your wishes are honored and your assets are protected for future generations. If you live in Tennessee, working with a qualified estate planning attorney is the best way to navigate this...
What Is Elder Law? Essential Legal Services for Seniors
What is elder law? Learn how elder law attorneys in Nashville, TN help seniors with estate planning, Medicaid, guardianship & more. Protect your future today!
Finding the Right Elder Care Lawyer in Nashville: Protect Your Family’s Future
As families in Nashville and throughout Tennessee navigate the complexities of aging, legal planning becomes essential to protecting assets, ensuring quality care, and maintaining financial stability. An elder care lawyer specializes in helping seniors and their...
Understanding Special Needs Trusts in Tennessee: A Comprehensive Guide
Planning for the future of a loved one with special needs can feel overwhelming, especially when considering their financial security and eligibility for government benefits. A Special Needs Trust (SNT) is a powerful legal tool that helps protect assets while ensuring...
What Is an Elder Law Attorney? Legal Services for Tennessee Families
What is an elder law attorney? Learn how Tennessee families can protect assets, plan for long-term care & navigate legal challenges with expert guidance.
Tennessee Asset Protection Trusts – Do You Need One?
Navigating Tennessee Asset Protection Trusts For many of us in the middle class- navigating Tennessee asset protection trusts can be hard to understand. For those who aren't multimillionaires but also don’t qualify for financial assistance—it’s crucial to think about...
Understanding the Costs: How Much Do Elder Law Attorneys Charge?
When considering elder law attorneys, especially in Nashville, Tennessee, and the surrounding areas, one of the most common concerns is understanding the associated costs. Elder law attorneys provide crucial services to seniors and their families, helping them...
When Is the Right Time to Consult an Elder Law Attorney?
Residents of Nashville, have you ever asked yourself, when should I hire an elder law attorney? Elder law encompasses a variety of areas tailored to the unique needs of our clients, including estate planning, Medicaid planning, Medicaid benefits, VA benefits,...
Seniors in Nashville, TN: Don’t Put Off Seeing an Estate Planning Attorney
There are times when seniors in Nashville, TN, Brentwood, Franklin, or other nearby suburbs need to talk to an estate planning lawyer. It’s essential to ensure that a proper plan is in place that will provide for (1) decision-making on financial and health care...
Why Revocable Living Trusts Are a Smart Estate Planning Tool in Nashville, TN
Revocable Living Trusts in Nashville, Tennessee When it comes to estate planning, many Tennesseans believe that a will is all they need to ensure their loved ones are cared for after they pass. However, it's essential to consider key questions regarding the...
Estate Planning in Tennessee
Have you done your estate planning? Have you worked with a lawyer to develop an estate plan but realize it’s out of date? You might know what you need to do, but the task often gets delayed. In the United States, we’ve become particularly good at putting off planning...
How Does TennCare in Tennessee Work?
How Does TennCare Work? In Tennessee, TennCare serves as a rebranded version of Medicaid. Originally established by President Lyndon Johnson in 1965, Medicaid aims to offer health coverage to low-income families and individuals, encompassing children, parents,...
Primer for a Working Parent in Tennessee
By Barbara Moss Published June 13, 1991, The Tennessean This is the article I wish someone had written 15 years ago when I began combining career and parenthood. I had my first child in 1977 when I was...
Understanding Elder Law and Life Care Planning in Tennessee
Considering elder law and life care planning in Nashville is essential for ensuring the well-being, financial stability, and legal protection of older individuals and their families. It allows for a proactive approach to addressing potential challenges associated with...
What is a Trust and How Does It Work?
Manage & pass down assets with a revocable or irrevocable trust. You may have heard about “trusts” over the years, but very few nonlawyers actually know what they are. The History of Trusts The use of trusts originated in the Middle Ages when English knights...
The Problem with Do-It-Yourself Estate Planning
Protect your family and your wishes by consulting an experienced estate planning attorney in Nashville, TN. Ever since the introduction of estate planning forms online, more and more people have bought into the idea that they could draft their own estate planning...
The Costs of Dementia for the Patient and Family
Life care planning programs that include care coordination provide support for family members with dementia. The Alzheimer’s Association reports that one in nine Americans age 65 or older currently has Alzheimer’s. With the baby boomer generation aging and people...
Medicaid Planning: When to Seek an Attorney
If a family member goes into a nursing home, contact an attorney to discuss your Medicaid planning options. What would happen if your spouse or a parent went into a nursing home? How would you or they pay for it? The average cost for a semi-private room in a...
Probate in Tennessee
Secure your future with experienced probate attorneys in Nashville, TN. Probate Solidifies The Last Will & Testament Many lay people believe that a last will and testament controls what happens from the moment the person who signed the will (“the testator”) passes...
Probate for Business Owners in Tennessee
Learn how estate planning with a probate lawyer helps provide a clear succession plan as a business owner. How Can a Probate Lawyer Help? If you own a family business, much of your wealth may be directly connected to your business activities. If this is the case,...
Long-Term Care Insurance & Estate Planning
Work with an estate planning attorney to determine the best long-term care decisions for your family. So many of us are failing to plan ahead for the inevitability of death and decline. I can understand and sympathize, but many of us are missing the chance to make our...
Plan for the Future with Power of Attorney
Learn what a power of attorney is, when you need it, and how it can protect your family. Protect Loved Ones with Power of Attorney I recently met with a senior couple who had lived a fruitful and financially successful life together. They obviously cared for each...
Conservatorships in Nashville, TN
Why we recommend avoiding a conservatorship and how a conservatorship attorney can help your family. Avoiding a Conservatorship in Tennessee Under Tennessee law, when someone becomes incapacitated, a family member or other interested adult must go to probate court and...
The Latest Scam Involves Medicaid Cards
Beginning April 2018, Medicare will begin the year-long process of issuing new Medicare cards. The new card will have a unique Medicare number listed, not your social security number. You will NOT have to do anything to receive this new card. This change...
Avoid the Family Fight
You love your family. We all want our families to get along, grow together, and to lean on each other after we are gone. I've never had a client who wanted his or her death to cause a fight or even lasting enmity among heirs. All too often, however, that is exactly...
You Don’t Have to Give Your Doctor Your Social Security Number
While no cybercriminal worth his salt would turn down a chance to get his hands on your credit card information, there’s an even bigger prize: your Social Security number, which cybersecurity experts say is now the single most valuable piece of information in terms of...
Tax Season Scams
Crimes against the elderly continue to skyrocket each year, as criminals continue to find more ways to carry out both new and old scams. This information which we received courtesy of the Council on Aging in Nashville is particularly timely. Last month, the IRS...
Yoga Can Prevent Falls among the Elderly
I'm a happy yoga practitioner, so I was glad to see this news: People who do hatha yoga report improved balance, but only now has yoga’s impact on falls received rigorous study. Now, University of Wisconsin–Madison professor of family medicine Irene Hamrick reports...
Tips for Avoiding Charity Scams
(This article comes courtesy of Council on Aging, a wonderful organization in Nashville.) As people all over the world try to help survivors of Hurricanes Harvey and Irma with donations of food and water, clothes, shelter and money, we want to remind you to be aware...
Elder Law Attorneys Resisting Mandatory Pre-Dispute Arbitration Agreements
The National Association of Elder Law Attorneys (NAELA) has joined with other stakeholders to resist a new regulation proposed by the Center for Medicare and Medicaid Services to allow nursing homes to require residents to enter into an agreement to forego their day...
Want to Live a Longer and Healthier Life? Make Friends!
According to a recent article in the New York Times, quoting the Harvard Women's Health Study, "Dozens of studies have shown that people who have satisfying relationships with family, friends, and their community are happier, have fewer health problems, and live...
Elder Law Attorneys and Other Health Groups Are Worried about Your Healthcare
The National Association of Elder Law Attorneys, "NAELA," which is in no way a partisan organization, is reporting this morning as follows: "Health care groups are decrying Republican senators for closing their doors to the public as they write legislation repealing...
If You Are Middleclass, You May Think You Don’t Need Medicaid. Think Again.
An article in the New York Times this morning explains what happens if your mother, who has $100,000, goes into a nursing home. If she lives two years or more, she will run out of money and will need Medicaid to stay in a nursing home. Cuts to Medicaid will...
Will the Plans You Make for Treatment at the End of Your Life be Ignored?
We encourage our clients to make plans for their healthcare by executing two documents: 1) a healthcare power of attorney which appoints someone to make decisions 2) an advance directive that lets our clients choose what end of life care, such as CPR and tube feeding,...
Poem by a Nashville Physician
Brenda Butka is a Nashville physician and has written this beautiful poem about the difficulty of letting go. Do Not Resuscitate Brenda Butka, MD Author Affiliations JAMA. 2012;308(16):1613. doi:10.1001/2012.jama.11596 I can say your father is dying. I can say...
What Do You Have in Common with Marlon Brando and Whitney Houston?
You might be surprised to find out! Check out this website for the answer. AARP article on celebrity estate planning mistakes
Not Things, but Peace of Mind as Your Gift
This year for the holidays, why not give yourself and your loved ones a little peace of mind? Wouldn’t your children be relieved to be told that you’ve done the planning so that if you become incapacitated, you have appointed perhaps a spouse and then a child to help...
What happens when all the Baby Boomers retire?
The number of Americans ages 65 and older is currently thought to be somewhere around 46 million. This number is projected to more than double to over 98 million by 2060, and the 65-and-older age group’s share of the total population will rise to nearly 24 percent...
Hearing Loss and Dementia
According to the CDC, nearly 20 percent of those from ages 40 to 69, and 43 percent of those 70 and older, have some degree of hearing loss. Yet among people over 50 with hearing loss, only one in seven uses hearing aids. Hearing loss is not just an inconsequential...
Another Example of Elder Abuse
Unfortunately, there are many predators out there who target seniors. Saddest of all are the family members. In California, an elderly couple is facing eviction because of the actions of their grandson. Helen and Hank Kawecki, 87 and 88, are in the process of packing...
Seniors Are Struggling with Drug Costs
A recent article in Consumer Reports contains disturbing information about the costs of prescription medicine for seniors. Seniors are more likely to need multiple medications. A survey conducted by Consumer Reports found that three-fourths of Americans 65 and older...
The Consequences of Failing to Plan for Dementia
Here are the statistics on dementia: according to the Alzheimer’s Foundation (Alzheimer’s is the most prevalent form of dementia), one in 9 Americans 65 and older, and one in 3 Americans 85 and older, has Alzheimer’s. Realistically, you should take dementia into...
Don’t Wait Too Long to Plan for Disability
I often receive calls from a family member whose loved one is receiving care at home, in an assisted living facility or in a nursing home and the call begins something like this: "I've used all of Mom's (or Dad's) money (to pay for health care) and I thought I should...
The First Step in the Probate Process: After Your Loved One Dies, How Do You Find the Will?
There's a little known statute in Tennessee that allows family members who are searching for the will of a loved one who has died to have access to the safe deposit box. Under Tennessee Code Section 45-2-905, when the sole or last surviving lessee of a safe deposit...
“Avoiding Probate” in Tennessee
All too often, I hear from people who are interested in estate planning documents and want to "avoid probate." Often, they don't know what probate involves or why they want to avoid it. Probate can be avoided by use of a revocable trust or "living trust" instead of...
What Does it Mean to be Chosen as a “Super Lawyer”
I've been recognized by Super Lawyers Magazine of the Mid South as a Super Lawyer in the area of Elder Law. According to Super Lawyers Magazine: "Peer nominations and evaluations are combined with third party research. Each candidate is evaluated on 12 indicators of...
New Insight Into Helping the Elderly
For many caregivers, one of the most difficult aspects of their seemingly thankless jobs is the ingratitude of the family members for whom they are providing care. A friend and geriatric manager recently forwarded to me this article from The New York Times: New York...
Some Hope for Disabled Tennessee Residents Who Need Medicaid to Pay for Nursing Home Care
I have posted previously about elderly Tennessee residents who fail to qualify for Medicaid (called TennCare here in Tennessee) nursing home services because they receive a pre-admission evaluation ("PAE") with a score less than 9. A score of 9 is required to qualify...
Why Tennessee Elders Are Failing to Qualify for Medicaid
I've written on this topic before, but the situation can be so serious for those that are affected, I wanted to discuss it again. On July 1, 2012, the Tennessee Bureau of TennCare (Tennessee's version of Medicaid) adopted new guidelines to determine who would be...
Treating Your Children Equally in Estate Planning
Many parents express a desire to leave their assets to their children in equal shares. In my opinion, that should be the default position for parents with more than one child. After all, who wants to convey a message to a child that he or she is less valued? I joke...
Who Pays In Tennessee When Your Mom Or Dad (Or Spouse) Needs Long Term Care?
A professor of economics at the New School for Social Research estimated that 75 percent of Americans who were nearing retirement in 2010 had less than $30,000 in their retirement accounts. The percentages have not gotten any better since 2010. At the same time, a...
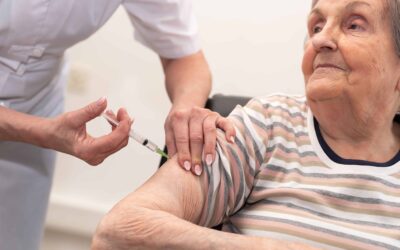
Seniors in Tennessee Should Get the Flu Vaccine
It's October, time to be thinking about getting the Flu Vaccine. There are many sites in Nashville, Tennessee set up to give flu shots on demand this year. For seniors, this is especially important, since flu season can be deadly. Ninety percent (90%) of deaths and...
Which is Right for You: Will or Revocable Trust?
Hopefully, there are readers who are wondering about a plan to dispose of their assets and take care of their family members. You may have seen newspaper advertisements or have been to seminars where revocable trusts, sometimes called "living trusts," are touted. ...
How Does Estate Recovery Work in Tennessee?
For many seniors, their primary asset and sometimes their only asset is their home. They are concerned that they will have to sign away their homes to qualify for Medicaid, called TennCare here in Tennessee. They worry that the state will file a lien...
An Article that All Seniors and Children of Aging Parents Should Read
I recently found myself advising a client whose mother had just entered an assisted living facility to read an article written by Michael Wolff called "A Life Worth Ending," published about a year ago in New York Magazine. Here's a link: Parents' challenges in...
Emergency Conservatorships in Tennessee
Until July, 2013, there was no statute in Tennessee governing how and under what circumstances a court could appoint an emergency conservator for a person with a disability (called the "respondent" in this type of proceeding). At the same time, there...
Save the Stories of Your Relatives!
This is not a post about legal issues, but rather about a hobby of mine--interviewing all the relatives in my family, my husband's family, my ex-husband's family, etc.--in an attempt to preserve the stories that family members know and that will be gone...
Why Some Seniors in Tennessee Are Failing to Qualify for Medicaid
Medicaid (known as TennCare in Tennessee) is a federal-state partnership program that pays for about half of long term care costs in America (excluding the costs of in-home care provided by families). Federal law sets out the limitations on assets that determine...
Seniors Need to Plan for Housing
Each week I encounter someone who has promised a family member that he or she would never be placed in a nursing home. Other than extracting and making that promise, families have often done very little planning for the housing needs of senior family members. This...
How Elder Law Found Me
When I graduated from law school in 1977, there was no subject called "Elder Law." To be honest, I probably would not have taken that course, anyway. I was the first woman hired by a big, downtown law firm. I wanted to work in litigation, and I don't believe that I...
How Will I Pay for Nursing Home Care in Tennessee?
Studies have confirmed that people say they fear public speaking more than death. I understand the instant humiliation of public speaking. But I secretly believe that these studies are more about the belief that we are not going to die, or have a stroke, break a...
Early Action Can Prevent a Family Crisis
Life care planning helps Nashville and Middle Tennessee families protect care, finances, and peace of mind before aging challenges turn into a stressful crisis at home.
Estate Planning Mistakes That Can Cost Nashville TN Families Thousands
Key Takeaways Many estate planning mistakes are not discovered until a medical emergency, death, or probate dispute occurs. A will alone may not fully protect assets or help families avoid probate in Tennessee. Outdated beneficiaries, missing powers of attorney, and...
Protecting Your Home and Savings with Estate Planning in East Brentwood
Estate planning helps East Brentwood families protect their homes, savings, beneficiaries, and long-term wishes. A comprehensive estate plan can reduce probate complications and help loved ones avoid unnecessary court involvement. Wills, trusts, powers of attorney,...
How a Disability Attorney in Franklin, TN Helps Protect Your Benefits and Future
Key Takeaways A disability attorney in Franklin, TN, handles every stage of a Social Security disability claim, from the initial application through the appeals process. Social Security Disability Insurance requires enough work credits from your work history;...
What a Medicaid Planning Attorney Does for Nashville Seniors and Families
Key Takeaways: A Medicaid planning attorney helps families qualify for Medicaid while protecting assets and avoiding costly mistakes. Medicaid rules in Tennessee are complex, highly specific, and easy to misunderstand without professional guidance. Long-term...
Writing Your Will in Tennessee? Why Hiring a Last Will Lawyer Is Essential
Key Takeaways Tennessee wills must meet strict signing and witness rules DIY wills often lead to costly mistakes and disputes Estate planning lawyers provide personalized, legally valid documents Regularly update your will after major life changes Wills alone may not...
How to Find the Best Elder Law and Estate Planning Attorneys in Nashville, TN
Key Takeaways The best attorneys in Nashville, TN, combine legal skill with genuine compassion. Choose a lawyer who focuses on elder law or estate planning every day. Working with a local Nashville attorney helps you plan with Tennessee laws and resources in mind....
What Is a Medicaid Asset Protection Trust and How Does It Work in Tennessee?
Key Takeaways A Medicaid Asset Protection Trust helps families protect savings and property while meeting Medicaid’s asset limit for long-term care. Because it’s an irrevocable trust, any assets transferred into it must be planned well in advance. Tennessee has a...
Hearing Loss and Dementia: How Early Intervention Protects Health and Independence
Key Takeaways Hearing loss is common in older adults and linked to a higher risk of dementia. Early diagnosis and treatment can help protect memory and mental clarity. Regular hearing evaluations after age 50 are essential for healthy aging. Untreated hearing loss can...
Are Children Responsible for Their Parents’ Debt After Death? A Guide for Nashville Families
Key Takeaways In Tennessee, children are not personally responsible for unpaid debts in a parent’s name alone. Debts are settled through probate and paid from the parents’ estate before any assets are distributed to the heirs. Children may only be liable for debts...
How to Prove Undue Influence in a Tennessee Will or Trust Case
Key Takeaways Undue influence occurs when someone manipulates a vulnerable person to change a will or trust. Proving undue influence requires evidence of control, pressure, or unfair persuasion. Tennessee law looks at relationships, suspicious circumstances, and...
Recorded Deed Notices: Protecting Yourself from Property Scams for Tennessee Residents
Key Takeaways A recorded deed notice helps confirm that your property ownership is secure. Scammers often target seniors with fake notices or fraudulent property filings. Tennessee homeowners can protect themselves by verifying official notices and monitoring records....
A Guide to Tennessee Veterans Benefits: What You May Be Missing
Key Takeaways: Many Tennessee veterans and their spouses are missing out on state and federal benefits to which they’re eligible. Available programs include VA healthcare, Aid & Attendance, and burial benefits. Surviving spouses may also be eligible for monthly...
Irrevocable Trusts Explained: Protecting Assets with the Right Legal Guidance
Key Takeaways: Irrevocable trusts can shield assets from long-term care costs and estate taxes. These trusts are not easily changed; professional guidance is key. An experienced irrevocable trust attorney helps ensure your wishes are protected. Families across Middle...
Paranoia and Cognitive Decline in the Elderly: What Nashville Families Should Know
Key Takeaways: Paranoia in elderly individuals may signal underlying cognitive decline. It can be caused by dementia, medication side effects, or loss of hearing or vision. Early legal planning can protect your loved one’s well-being and finances. Local attorneys can...
Estate Planning in Hendersonville, TN: How a Local Attorney Can Help
Key Takeaways: Estate planning is more than a will; it's about protecting your loved ones and your legacy. Local attorneys in Hendersonville, TN, are well-versed in state laws and understand the community's specific needs. Services may include wills, powers of...
Elder Abuse in Tennessee: What Families Need to Know
Key Takeaways: Elder abuse in Tennessee includes physical, emotional, financial, and neglect-related harm. Warning signs include mood changes, unexplained injuries, and missing money. Tennessee law requires certain professionals to report suspected elder abuse. Legal...
Planning Ahead: What a Wills and Trust Attorney Near You in Nashville, TN Can Offer
Need a wills and trust attorney near Nashville, TN? Learn how estate planning in Tennessee can protect your family, assets, and legacy with expert legal support.
Navigating Tennessee Medicaid for Seniors: A Step-by-Step Guide
Explore this guide by Elder Law of Nashville on Tennessee Medicaid for seniors. Learn eligibility, benefits, and how to apply.
Finding the Best Nashville Estate Planning Attorney: Protect Your Legacy & Loved Ones
You’ve undoubtedly been planning for the future your whole life, but there comes a time when such planning doesn’t include you in that future. Instead, such planning helps ensure the best for your family after you die. Estate planning ensures that your assets are...
Understanding Medicaid Eligibility in Tennessee: What You Need to Know for 2025
Elder Law of Nashville details what you need to know about Medicaid eligibility in Tennessee and how to navigate TennCare requirements.
Choosing the Best Elder Lawyers in Nashville: Key Factors to Consider for Your Family’s Protection
Finding an elder lawyer in the Nashville, Tennessee, area is as easy as typing “elder lawyer near me” into your Internet search engine. For a more comprehensive search, you can get listings of Nashville-area elder lawyers from any legal organizations that profile,...
Why You Need an Estate Planning Attorney in TN: Protecting Your Assets and Legacy
Estate planning is one of the most crucial steps you can take to ensure that your wishes are honored and your assets are protected for future generations. If you live in Tennessee, working with a qualified estate planning attorney is the best way to navigate this...
What Is Elder Law? Essential Legal Services for Seniors
What is elder law? Learn how elder law attorneys in Nashville, TN help seniors with estate planning, Medicaid, guardianship & more. Protect your future today!
Finding the Right Elder Care Lawyer in Nashville: Protect Your Family’s Future
As families in Nashville and throughout Tennessee navigate the complexities of aging, legal planning becomes essential to protecting assets, ensuring quality care, and maintaining financial stability. An elder care lawyer specializes in helping seniors and their...
Understanding Special Needs Trusts in Tennessee: A Comprehensive Guide
Planning for the future of a loved one with special needs can feel overwhelming, especially when considering their financial security and eligibility for government benefits. A Special Needs Trust (SNT) is a powerful legal tool that helps protect assets while ensuring...
What Is an Elder Law Attorney? Legal Services for Tennessee Families
What is an elder law attorney? Learn how Tennessee families can protect assets, plan for long-term care & navigate legal challenges with expert guidance.
Tennessee Asset Protection Trusts – Do You Need One?
Navigating Tennessee Asset Protection Trusts For many of us in the middle class- navigating Tennessee asset protection trusts can be hard to understand. For those who aren't multimillionaires but also don’t qualify for financial assistance—it’s crucial to think about...
Understanding the Costs: How Much Do Elder Law Attorneys Charge?
When considering elder law attorneys, especially in Nashville, Tennessee, and the surrounding areas, one of the most common concerns is understanding the associated costs. Elder law attorneys provide crucial services to seniors and their families, helping them...
When Is the Right Time to Consult an Elder Law Attorney?
Residents of Nashville, have you ever asked yourself, when should I hire an elder law attorney? Elder law encompasses a variety of areas tailored to the unique needs of our clients, including estate planning, Medicaid planning, Medicaid benefits, VA benefits,...
Seniors in Nashville, TN: Don’t Put Off Seeing an Estate Planning Attorney
There are times when seniors in Nashville, TN, Brentwood, Franklin, or other nearby suburbs need to talk to an estate planning lawyer. It’s essential to ensure that a proper plan is in place that will provide for (1) decision-making on financial and health care...
Why Revocable Living Trusts Are a Smart Estate Planning Tool in Nashville, TN
Revocable Living Trusts in Nashville, Tennessee When it comes to estate planning, many Tennesseans believe that a will is all they need to ensure their loved ones are cared for after they pass. However, it's essential to consider key questions regarding the...
Estate Planning in Tennessee
Have you done your estate planning? Have you worked with a lawyer to develop an estate plan but realize it’s out of date? You might know what you need to do, but the task often gets delayed. In the United States, we’ve become particularly good at putting off planning...
How Does TennCare in Tennessee Work?
How Does TennCare Work? In Tennessee, TennCare serves as a rebranded version of Medicaid. Originally established by President Lyndon Johnson in 1965, Medicaid aims to offer health coverage to low-income families and individuals, encompassing children, parents,...
Primer for a Working Parent in Tennessee
By Barbara Moss Published June 13, 1991, The Tennessean This is the article I wish someone had written 15 years ago when I began combining career and parenthood. I had my first child in 1977 when I was...
Understanding Elder Law and Life Care Planning in Tennessee
Considering elder law and life care planning in Nashville is essential for ensuring the well-being, financial stability, and legal protection of older individuals and their families. It allows for a proactive approach to addressing potential challenges associated with...
What is a Trust and How Does It Work?
Manage & pass down assets with a revocable or irrevocable trust. You may have heard about “trusts” over the years, but very few nonlawyers actually know what they are. The History of Trusts The use of trusts originated in the Middle Ages when English knights...
The Problem with Do-It-Yourself Estate Planning
Protect your family and your wishes by consulting an experienced estate planning attorney in Nashville, TN. Ever since the introduction of estate planning forms online, more and more people have bought into the idea that they could draft their own estate planning...
The Costs of Dementia for the Patient and Family
Life care planning programs that include care coordination provide support for family members with dementia. The Alzheimer’s Association reports that one in nine Americans age 65 or older currently has Alzheimer’s. With the baby boomer generation aging and people...
Medicaid Planning: When to Seek an Attorney
If a family member goes into a nursing home, contact an attorney to discuss your Medicaid planning options. What would happen if your spouse or a parent went into a nursing home? How would you or they pay for it? The average cost for a semi-private room in a...
Probate in Tennessee
Secure your future with experienced probate attorneys in Nashville, TN. Probate Solidifies The Last Will & Testament Many lay people believe that a last will and testament controls what happens from the moment the person who signed the will (“the testator”) passes...
Probate for Business Owners in Tennessee
Learn how estate planning with a probate lawyer helps provide a clear succession plan as a business owner. How Can a Probate Lawyer Help? If you own a family business, much of your wealth may be directly connected to your business activities. If this is the case,...
Long-Term Care Insurance & Estate Planning
Work with an estate planning attorney to determine the best long-term care decisions for your family. So many of us are failing to plan ahead for the inevitability of death and decline. I can understand and sympathize, but many of us are missing the chance to make our...
Plan for the Future with Power of Attorney
Learn what a power of attorney is, when you need it, and how it can protect your family. Protect Loved Ones with Power of Attorney I recently met with a senior couple who had lived a fruitful and financially successful life together. They obviously cared for each...
Conservatorships in Nashville, TN
Why we recommend avoiding a conservatorship and how a conservatorship attorney can help your family. Avoiding a Conservatorship in Tennessee Under Tennessee law, when someone becomes incapacitated, a family member or other interested adult must go to probate court and...
The Latest Scam Involves Medicaid Cards
Beginning April 2018, Medicare will begin the year-long process of issuing new Medicare cards. The new card will have a unique Medicare number listed, not your social security number. You will NOT have to do anything to receive this new card. This change...
Avoid the Family Fight
You love your family. We all want our families to get along, grow together, and to lean on each other after we are gone. I've never had a client who wanted his or her death to cause a fight or even lasting enmity among heirs. All too often, however, that is exactly...
You Don’t Have to Give Your Doctor Your Social Security Number
While no cybercriminal worth his salt would turn down a chance to get his hands on your credit card information, there’s an even bigger prize: your Social Security number, which cybersecurity experts say is now the single most valuable piece of information in terms of...
Tax Season Scams
Crimes against the elderly continue to skyrocket each year, as criminals continue to find more ways to carry out both new and old scams. This information which we received courtesy of the Council on Aging in Nashville is particularly timely. Last month, the IRS...
Yoga Can Prevent Falls among the Elderly
I'm a happy yoga practitioner, so I was glad to see this news: People who do hatha yoga report improved balance, but only now has yoga’s impact on falls received rigorous study. Now, University of Wisconsin–Madison professor of family medicine Irene Hamrick reports...
Tips for Avoiding Charity Scams
(This article comes courtesy of Council on Aging, a wonderful organization in Nashville.) As people all over the world try to help survivors of Hurricanes Harvey and Irma with donations of food and water, clothes, shelter and money, we want to remind you to be aware...
Elder Law Attorneys Resisting Mandatory Pre-Dispute Arbitration Agreements
The National Association of Elder Law Attorneys (NAELA) has joined with other stakeholders to resist a new regulation proposed by the Center for Medicare and Medicaid Services to allow nursing homes to require residents to enter into an agreement to forego their day...
Want to Live a Longer and Healthier Life? Make Friends!
According to a recent article in the New York Times, quoting the Harvard Women's Health Study, "Dozens of studies have shown that people who have satisfying relationships with family, friends, and their community are happier, have fewer health problems, and live...
Elder Law Attorneys and Other Health Groups Are Worried about Your Healthcare
The National Association of Elder Law Attorneys, "NAELA," which is in no way a partisan organization, is reporting this morning as follows: "Health care groups are decrying Republican senators for closing their doors to the public as they write legislation repealing...
If You Are Middleclass, You May Think You Don’t Need Medicaid. Think Again.
An article in the New York Times this morning explains what happens if your mother, who has $100,000, goes into a nursing home. If she lives two years or more, she will run out of money and will need Medicaid to stay in a nursing home. Cuts to Medicaid will...
Will the Plans You Make for Treatment at the End of Your Life be Ignored?
We encourage our clients to make plans for their healthcare by executing two documents: 1) a healthcare power of attorney which appoints someone to make decisions 2) an advance directive that lets our clients choose what end of life care, such as CPR and tube feeding,...
Poem by a Nashville Physician
Brenda Butka is a Nashville physician and has written this beautiful poem about the difficulty of letting go. Do Not Resuscitate Brenda Butka, MD Author Affiliations JAMA. 2012;308(16):1613. doi:10.1001/2012.jama.11596 I can say your father is dying. I can say...
What Do You Have in Common with Marlon Brando and Whitney Houston?
You might be surprised to find out! Check out this website for the answer. AARP article on celebrity estate planning mistakes
Not Things, but Peace of Mind as Your Gift
This year for the holidays, why not give yourself and your loved ones a little peace of mind? Wouldn’t your children be relieved to be told that you’ve done the planning so that if you become incapacitated, you have appointed perhaps a spouse and then a child to help...
What happens when all the Baby Boomers retire?
The number of Americans ages 65 and older is currently thought to be somewhere around 46 million. This number is projected to more than double to over 98 million by 2060, and the 65-and-older age group’s share of the total population will rise to nearly 24 percent...
Hearing Loss and Dementia
According to the CDC, nearly 20 percent of those from ages 40 to 69, and 43 percent of those 70 and older, have some degree of hearing loss. Yet among people over 50 with hearing loss, only one in seven uses hearing aids. Hearing loss is not just an inconsequential...
Another Example of Elder Abuse
Unfortunately, there are many predators out there who target seniors. Saddest of all are the family members. In California, an elderly couple is facing eviction because of the actions of their grandson. Helen and Hank Kawecki, 87 and 88, are in the process of packing...
Seniors Are Struggling with Drug Costs
A recent article in Consumer Reports contains disturbing information about the costs of prescription medicine for seniors. Seniors are more likely to need multiple medications. A survey conducted by Consumer Reports found that three-fourths of Americans 65 and older...
The Consequences of Failing to Plan for Dementia
Here are the statistics on dementia: according to the Alzheimer’s Foundation (Alzheimer’s is the most prevalent form of dementia), one in 9 Americans 65 and older, and one in 3 Americans 85 and older, has Alzheimer’s. Realistically, you should take dementia into...
Don’t Wait Too Long to Plan for Disability
I often receive calls from a family member whose loved one is receiving care at home, in an assisted living facility or in a nursing home and the call begins something like this: "I've used all of Mom's (or Dad's) money (to pay for health care) and I thought I should...
The First Step in the Probate Process: After Your Loved One Dies, How Do You Find the Will?
There's a little known statute in Tennessee that allows family members who are searching for the will of a loved one who has died to have access to the safe deposit box. Under Tennessee Code Section 45-2-905, when the sole or last surviving lessee of a safe deposit...
“Avoiding Probate” in Tennessee
All too often, I hear from people who are interested in estate planning documents and want to "avoid probate." Often, they don't know what probate involves or why they want to avoid it. Probate can be avoided by use of a revocable trust or "living trust" instead of...
What Does it Mean to be Chosen as a “Super Lawyer”
I've been recognized by Super Lawyers Magazine of the Mid South as a Super Lawyer in the area of Elder Law. According to Super Lawyers Magazine: "Peer nominations and evaluations are combined with third party research. Each candidate is evaluated on 12 indicators of...
New Insight Into Helping the Elderly
For many caregivers, one of the most difficult aspects of their seemingly thankless jobs is the ingratitude of the family members for whom they are providing care. A friend and geriatric manager recently forwarded to me this article from The New York Times: New York...
Some Hope for Disabled Tennessee Residents Who Need Medicaid to Pay for Nursing Home Care
I have posted previously about elderly Tennessee residents who fail to qualify for Medicaid (called TennCare here in Tennessee) nursing home services because they receive a pre-admission evaluation ("PAE") with a score less than 9. A score of 9 is required to qualify...
Why Tennessee Elders Are Failing to Qualify for Medicaid
I've written on this topic before, but the situation can be so serious for those that are affected, I wanted to discuss it again. On July 1, 2012, the Tennessee Bureau of TennCare (Tennessee's version of Medicaid) adopted new guidelines to determine who would be...
Treating Your Children Equally in Estate Planning
Many parents express a desire to leave their assets to their children in equal shares. In my opinion, that should be the default position for parents with more than one child. After all, who wants to convey a message to a child that he or she is less valued? I joke...
Who Pays In Tennessee When Your Mom Or Dad (Or Spouse) Needs Long Term Care?
A professor of economics at the New School for Social Research estimated that 75 percent of Americans who were nearing retirement in 2010 had less than $30,000 in their retirement accounts. The percentages have not gotten any better since 2010. At the same time, a...
Seniors in Tennessee Should Get the Flu Vaccine
It's October, time to be thinking about getting the Flu Vaccine. There are many sites in Nashville, Tennessee set up to give flu shots on demand this year. For seniors, this is especially important, since flu season can be deadly. Ninety percent (90%) of deaths and...
Which is Right for You: Will or Revocable Trust?
Hopefully, there are readers who are wondering about a plan to dispose of their assets and take care of their family members. You may have seen newspaper advertisements or have been to seminars where revocable trusts, sometimes called "living trusts," are touted. ...
How Does Estate Recovery Work in Tennessee?
For many seniors, their primary asset and sometimes their only asset is their home. They are concerned that they will have to sign away their homes to qualify for Medicaid, called TennCare here in Tennessee. They worry that the state will file a lien...
An Article that All Seniors and Children of Aging Parents Should Read
I recently found myself advising a client whose mother had just entered an assisted living facility to read an article written by Michael Wolff called "A Life Worth Ending," published about a year ago in New York Magazine. Here's a link: Parents' challenges in...
Emergency Conservatorships in Tennessee
Until July, 2013, there was no statute in Tennessee governing how and under what circumstances a court could appoint an emergency conservator for a person with a disability (called the "respondent" in this type of proceeding). At the same time, there...
Save the Stories of Your Relatives!
This is not a post about legal issues, but rather about a hobby of mine--interviewing all the relatives in my family, my husband's family, my ex-husband's family, etc.--in an attempt to preserve the stories that family members know and that will be gone...
Why Some Seniors in Tennessee Are Failing to Qualify for Medicaid
Medicaid (known as TennCare in Tennessee) is a federal-state partnership program that pays for about half of long term care costs in America (excluding the costs of in-home care provided by families). Federal law sets out the limitations on assets that determine...
Seniors Need to Plan for Housing
Each week I encounter someone who has promised a family member that he or she would never be placed in a nursing home. Other than extracting and making that promise, families have often done very little planning for the housing needs of senior family members. This...
How Elder Law Found Me
When I graduated from law school in 1977, there was no subject called "Elder Law." To be honest, I probably would not have taken that course, anyway. I was the first woman hired by a big, downtown law firm. I wanted to work in litigation, and I don't believe that I...
How Will I Pay for Nursing Home Care in Tennessee?
Studies have confirmed that people say they fear public speaking more than death. I understand the instant humiliation of public speaking. But I secretly believe that these studies are more about the belief that we are not going to die, or have a stroke, break a...
When’s the Right Time to Create Your Estate Plan?
Visit our FAQs page to get answers to common questions or contact our team of elder law attorneys in Nashville today!